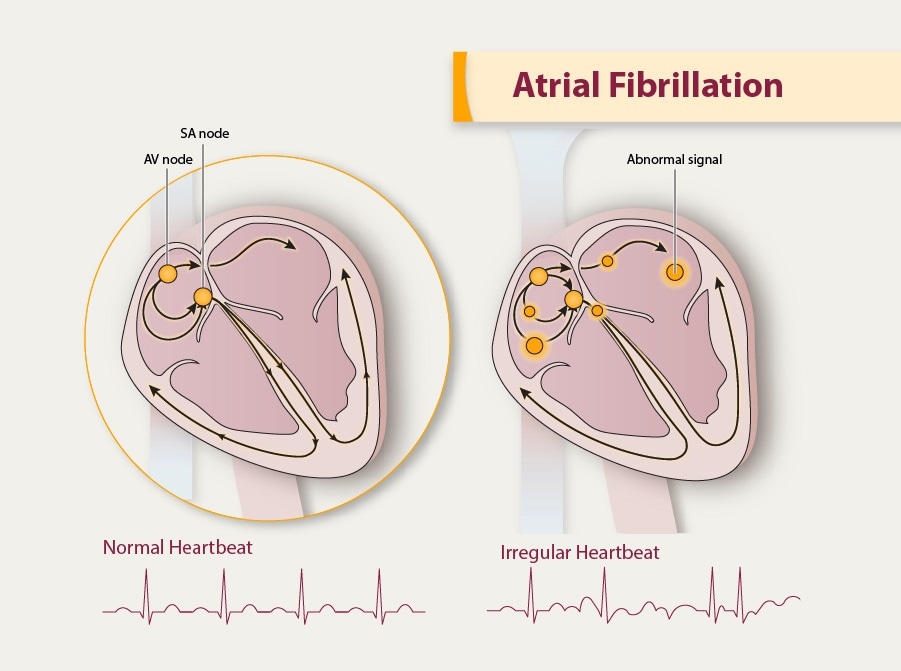
Accessory pathway conduction also can be present without apparent delta wave, in which case it is referred to as a concealed pathway. Accessory pathway electrical conduction can be manifested on electrocardiography (ECG) as a slurring (delta wave) of the initial portion of the QRS complex. If detected early and in the absence of systemic anticoagulation, iatrogenic cardiac tamponade caused by catheter perforation uncommonly is a life-threatening complication however, it does require the percutaneous insertion of a temporary subxiphoid pericardial drain if associated with hemodynamic compromise.ĪVRT, a category of supraventricular tachycardias under which Wolff-Parkinson-White syndrome falls, involves the transmission of electrical impulses across one or more extranodal (accessory) pathways. Introduction of catheters into the heart, with or without the delivery of ablative energy, uniformly carries the risk of cardiac perforation and possibly tamponade. Success and complication rates vary, depending on the individual arrhythmia ( Table 1 1 – 26). Once the patient's conduction system has been studied and the rhythm disturbance diagnosed, an ablation catheter is used to thermally destroy the pathogenic myocardial tissue underlying the arrhythmia's initiation or maintenance. Electrical stimulation is delivered to the myocardium via these catheters to characterize cardiac conduction and arrhythmias. The catheter tips are positioned at specific locations in the heart. 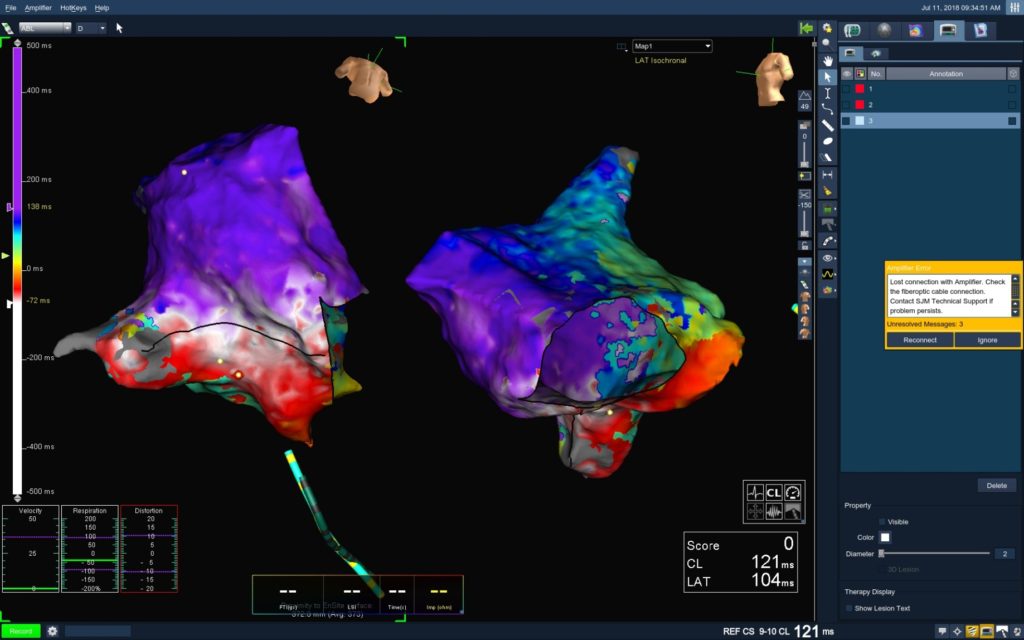
An electrophysiology study involves the percutaneous insertion of catheters into the femoral veins and often the internal jugular vein. Right atrium, if common variety of atrial flutterĬardiac perforation with tamponade heart block myocardial infarction thromboembolic events 20 – 22įirst-line therapy for poorly tolerated or recurrent episodes 1Ĭardiac perforation with tamponade phrenic nerve injury pulmonary vein stenosis thromboembolic events vascular complications 1, 25Īlternative to drug therapy for recurrent atrial fibrillation in symptomatic patients with minimal or no left atrial enlargement 23, 26Ĭatheter-based ablation of a cardiac arrhythmia is performed in an electrophysiology laboratory in conjunction with an electrophysiology study. Variable, left or right atrioventricular ring, septalĬomplete atrioventricular nodal block cardiac perforation with tamponade 1, 6, 13įirst-line therapy for symptoms, single or infrequent episodes, or with atrial fibrillation and rapid conduction 1 Incessant tachycardia symptomatic tachycardia tachycardia-mediated cardiomyopathy 1Ītrioventricular nodal reentrant tachycardiaĪtrioventricular nodal block, usually requiring pacemaker implantation 6, 7įirst-line therapy in patients willing and able to undergo catheter ablation 1Ītrioventricular reciprocating tachycardia Variable, anywhere in right or left atriumĪtrioventricular or sinus node dysfunction cardiac perforation with tamponade phrenic nerve injury 1 Complications associated with catheter ablation result from radiation exposure, vascular access (e.g., hematomas, cardiac perforation with tamponade), catheter manipulation (e.g., cardiac perforation with tamponade, thromboembolic events), or ablation energy delivery (e.g., atrioventricular nodal block). The complication rates for atrial fibrillation ablation range from 6 to 10 percent. Complication rates for supraventricular tachycardias and atrial flutter ablation are 0 to 8 percent. Catheter ablation effectiveness rates exceed 88 percent for atrioventricular nodal reentrant tachycardia, atrioventricular reciprocating tachycardia, and atrial flutter are greater than 86 percent for atrial tachycardia and range from 60 to 80 percent for atrial fibrillation. Catheter ablation of supraventricular tachycardias, atrial flutter, and atrial fibrillation offers patients high effectiveness rates, durable (and often permanent) therapeutic end points, and low complication rates. Depending on the arrhythmia, catheter ablation is a treatment option at initial diagnosis, when symptoms develop, or if medical therapy fails. Atrial fibrillation is a distinct entity classified separately. The term “supraventricular tachycardia” commonly refers to atrial tachycardia, atrioventricular nodal reentrant tachycardia, and atrioventricular reciprocating tachycardia, an entity that includes Wolff-Parkinson-White syndrome. The term “supraventricular arrhythmia” most often is used to refer to supraventricular tachycardias and atrial flutter. Supraventricular arrhythmias are relatively common, often persistent, and rarely life-threatening cardiac rhythm disturbances that arise from the sinus node, atrial tissue, or junctional sites between the atria and ventricles.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
